In the pursuit of deliberately becoming infected with Human Immunodeficiency Virus (HIV), bug chasers can feel anxious or even excited by the seroconversion process, along with feeling a number of other emotions. The symptoms experienced when seroconverting can vary from person to person, but are usually noticeable between 2 to 4 weeks after infection, which is known as the acute HIV infection stage. Typical symptoms include a fever, chills, muscle aches, swollen lymph nodes, rashes and fatigue, which can also be common symptoms for other health conditions.
A person might not become infected with HIV the first time they are exposed to the virus and the chances of success can vary considerably based on certain conditions. According to the Centers for Disease Control and Prevention (CDC), the estimated probability of acquiring HIV from an infected source for receptive bareback anal sex is 138 cases per 10,000 exposures, or 1.38% and for insertive bareback anal sex is 11 cases per 10,000 exposures, or 0.11%. While these numbers might seem extremely low for those who are trying to convert, there’s a number of factors that can affect these figures, such as the presence of sexually transmitted infections, acute and late-stage HIV infection and high viral load that can boost these numbers significantly.
The CDC offers an HIV risk estimator tool, so if you want to explore the risk factors more intricately, this estimator is an excellent tool and I have explored some of the factors that fall into the high risk and extreme risk categories using the data that’s currently available. I have only included the data that involves barebacking and no medication, whether this is PrEP for those who are HIV-negative or ART for those who are HIV-positive. There is a link to the estimator tool at the end of this article if you are interested in estimating particular scenarios including PrEP, condoms and ART, so you can tailor the data to your own needs to see the risk factors for additional situations.
| Risk Factor | Type of Sexual Position and Health Situation |
|---|---|
| 11 | Insertive anal sex + HIV |
| 29 | Insertive anal sex + HIV + STD |
| 77 | Insertive anal sex + HV + STD |
| 80 | Insertive anal sex + acute HIV infection |
| 138 | Receptive anal sex + HIV |
| 211 | Insertive anal sex + an STD + acute HIV infection |
| 366 | Receptive anal sex + HIV + STD |
| 1001 | Receptive anal sex + acute HIV infection |
| 2651 | Receptive anal sex + STD + acute HIV infection |
HIV is transmitted through body fluids, including blood, semen (cum), pre-seminal fluid (pre-cum), rectal fluids and for women, vaginal fluids and breast milk. These fluids must come into contact with a mucous membrane or damaged tissue or be directly injected into the bloodstream for transmission to occur. Most of the body’s surfaces feature dry skin, such as our arms and legs, so these surfaces don’t allow HIV to enter the body, unless a cut or sore is present, which is why HIV is primarily transmitted via particular areas of the body.
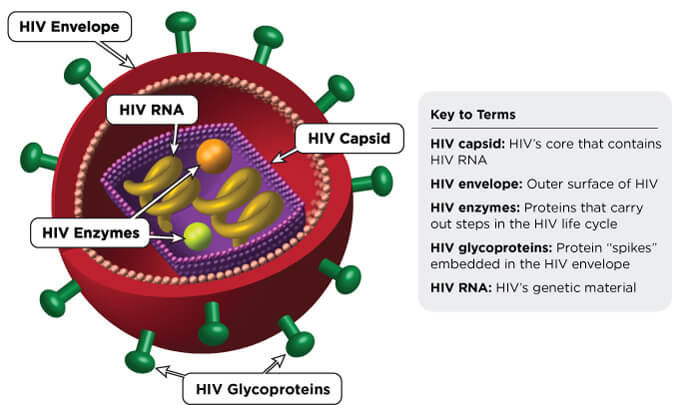
For HIV to enter our body, the virus needs a certain skin type, which is wet skin, known as mucous membranes. The mucous membranes are vulnerable to HIV and make it easier for HIV to enter the body. The wet skin involved in the transmission of HIV includes the foreskin and urethra on the penis, the anus and rectum, the mouth and throat and the cervix and vagina for women. Dry skin is covered with a protective layer of fibres that HIV cannot penetrate, unless there is a cut or sore present, but mucous membranes are not covered with the same protective layer of fibres, because it would hinder functionality, so this is the route HIV uses to enter our body.
You might be thinking that one load of high-viral cum flooding the anus through sexual intercourse might be enough to penetrate our body, which in some cases it is, but our body still has some tricks up its sleeve to fight off the virus before it enters the body. The mucous membranes are covered with a layer of cells that are tightly joined together and designed to help prevent germs from entering our body and causing an infection. The rectum has a single layer of cells, but the foreskin, urethra, mouth and vagina have multiple layers, which is why infection through receptive anal sex is more common than through vaginal or oral sex.
The mucous contains chemicals and antibodies that can kill germs, and under the cell layer, there’s a large concentration of immune cells responsible for attacking and killing germs that manage to find their way beyond the cell layer. If HIV can penetrate past the cell layer and immune cells below, then it has been able to successfully enter our body and at this point, the virus will find a host cell and start replicating within us. The protective layer can be weakened through sores or ulcers, which can be caused by sexually transmitted infections, such as herpes and syphilis or anal fissures and tears created by friction during sexual intercourse. The more HIV the cell layer is exposed to, the greater the chance that one or more particles will be able to find a way past the layer and enter the tissue below.
Once HIV has made it past the cell layer, a battle begins involving the body’s immune cells, which are present in the tissue below the cell layer. There are numerous types of immune cells in the mucous membranes and they each play a role in mounting an attack against HIV. Some of these cells are able to kill the virus, but HIV is able to infect one type of immune cell, which is the CD4 cell, which it then uses to make copies of itself and release more virus into the bloodstream. This battle lasts for 3 days, but you may not experience any symptoms associated with being infected with HIV at this point.
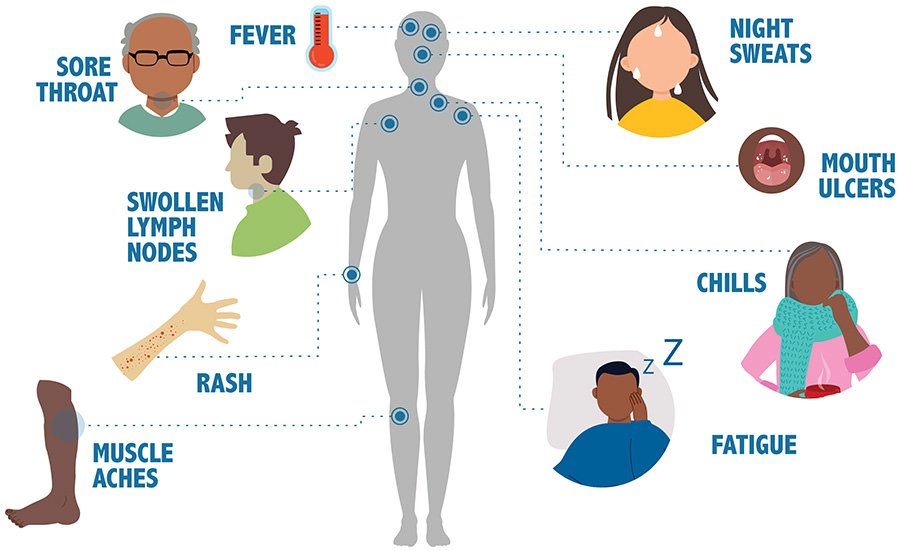
The symptoms present during the seroconversion process occur within 2 to 4 weeks after infection, but they go away after this period of time. The intensity of these symptoms, which some refer to as the ‘fuck flu’ can vary based on each person, with some becoming very sick from the symptoms, while others experience mild or even no symptoms at all. For those who do experience symptoms, these will go away after a while, even though the virus is still present in the body. This is not because the body has given up trying to defeat the HIV cells, but it’s instead because the body has figured out that it has only had partial success at eliminating the virus and it knows there will be an ongoing battle, so the body stops producing the responses that generate the fuck flu symptoms, as this is not beneficial for the body in the long run, otherwise the body wouldn’t function as well if these symptoms remained present in the long-term.
According to the latest CDC data available at this time (2019), 9% of gay and bisexual men in the United States with HIV had sex without using any HIV prevention strategy in the prior 12 months, which refers to having sex while not being virally suppressed with a partner whose HIV status was negative or unknown and where a condom was not used and the partner was not taking PrEP. Of the 36,801 estimated new HIV diagnoses in the United States for the same period, 25,552 (69%) were among gay and bisexual men, with gay and bisexual men aged between 13 and 34 making up the most new HIV diagnoses among all gay and bisexual men in the United States. In 2019, an estimated 1.2 million people had HIV in the United States, with 754,700 being gay and bisexual men, with 85 out of every 100 knowing their status, making 15% of people unaware of their HIV status.
Anal sex is the riskiest type of sex for acquiring or transmitting HIV, with receptive anal sex being 13 times as risky for getting HIV compared to insertive anal sex for the most common situations. For HIV-negative men who have an ulcerative sexually transmitted infection, their risk of contracting HIV increases by 2.65 times if they have anal sex with an HIV-positive partner. The risk of HIV transmission during acute infection is about 7.25 times the risk during the middle stage of HIV infection. This analysis has found that when looking at the standard chances of HIV infection, the level of risk can increase when an STI is present due to the layers of skin being damaged and creating an entry point for the virus and a high viral load also means the chances of infection can be even higher, which means there are some conditions that can increase the likelihood of HIV being transmitted more easily.
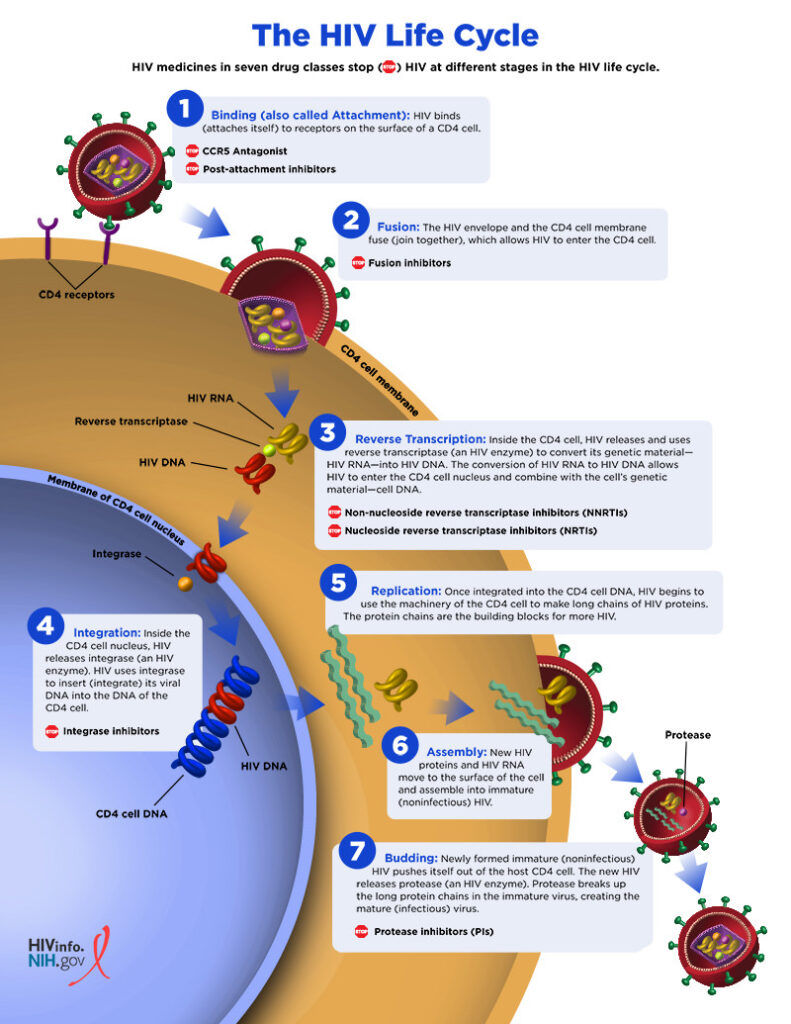
The first stage of HIV is known as acute HIV infection, which is when people have a large amount of HIV in their blood and are very contagious, with most people in this stage experiencing flu-like symptoms. The second stage of HIV is known as chronic infection and is also called asymptomatic HIV infection or clinical latency, where HIV is still active and continues to reproduce in the body. People may not have any symptoms or get sick during this phase, but they can still transmit HIV and this stage may last a decade or longer, but can also progress faster. The third and final stage of HIV is Acquired Immunodeficiency Syndrome (AIDS), which is the most severe stage and people with AIDS can have a high viral load and may easily transmit HIV to others and may have badly damaged immune systems and can experience serious illnesses. Without treatment, people with AIDS typically survive about 3 years.
There is no guaranteed infection rate and seroconversion symptoms can vary from person to person and a number of factors can result in a person becoming infected with HIV, which can be reliant on conditions such as viral load and the virus gaining access to the bloodstream after penetrating the body’s defence mechanisms. If a person has a poor immune system, this may mean that their body is not able to fight off the virus as effectively as someone who has a strong immune system. When it comes to HIV, one certainty is its unpredictability, and this is why the virus has been able to thrive for over 40 years with no current cure available, only a treatment that is able to manage the virus.
Information Sources and Further Reading:
Featured Photo: © Can Stock Photo / Spectral
Article ID: CC062
Version Control: 1.0 – May 6, 2023: Original article published.